How to implement digital health solutions in the Middle East

TL;DR:
- Building trust-first, coordinated digital ecosystems aligned with government mandates is crucial for success.
- Conducting readiness assessments helps identify gaps in leadership, infrastructure, and data before implementation.
- Interoperability and trust architecture are essential for sustainable digital health growth in the Middle East.
Healthcare executives across the Middle East are facing a defining moment. Fragmented legacy systems, rising patient volumes, and rapid national digital mandates are converging into a pressure point that demands more than good intentions. The organizations that will lead the next decade are not simply buying new software. They are building coordinated, trust-first digital ecosystems that align with government priorities and deliver measurable clinical outcomes. This guide gives you a practical, evidence-based roadmap covering readiness assessment, framework selection, execution best practices, and governance, so you can move from fragmented pilots to scaled, sustainable impact.
Table of Contents
- Assessing readiness: Digital maturity and leadership alignment
- Choosing the right frameworks: Structured approaches for success
- Executing implementation: Best practices and common pitfalls
- Securing outcomes: Data governance and trust architecture
- Why focusing on interoperability and trust drives long-term impact
- Partnering for digital health implementation success
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Start with readiness assessment | Evaluate digital maturity, leadership alignment, and compliance before launching any digital health project. |
| Use proven frameworks | Apply structured approaches like CFIR to guide each phase and ensure sustainable results. |
| Prioritize government alignment | Coordinate with national mandates and interoperability platforms for successful scaling. |
| Secure data and trust | Build robust governance and security-by-design to protect patient data and maintain trust. |
Assessing readiness: Digital maturity and leadership alignment
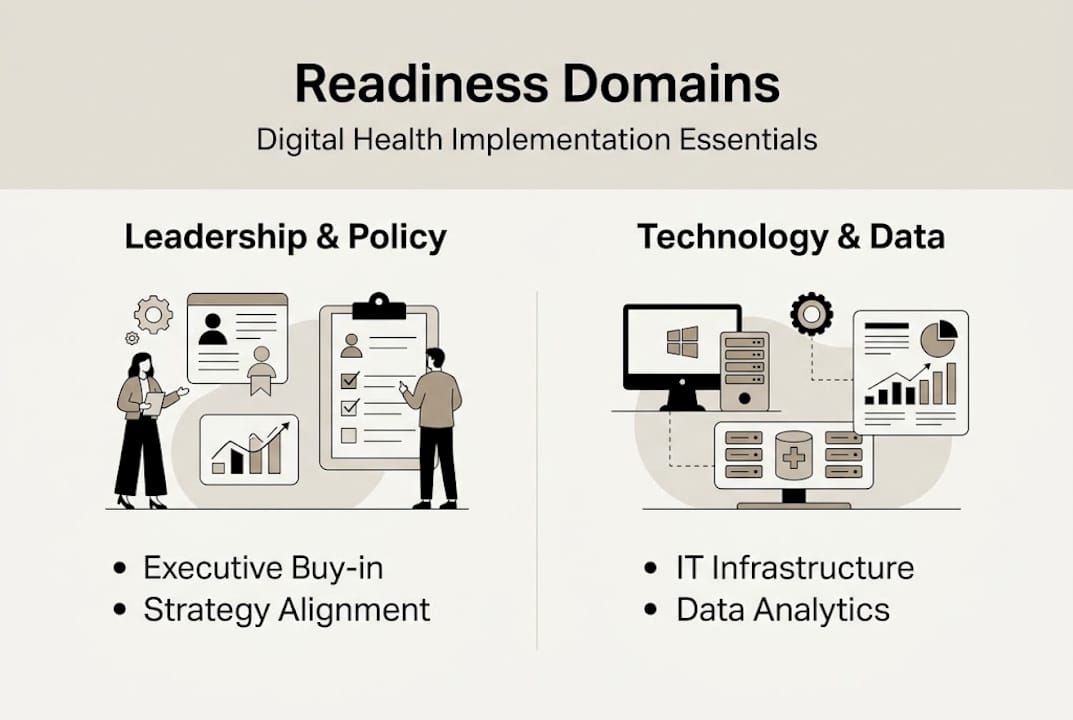
Before a single line of code is written or a vendor is selected, you need an honest picture of where your organization actually stands. Skipping this step is one of the most expensive mistakes healthcare IT leaders make. A structured digital maturity assessment evaluates readiness across three core domains: leadership and policy, infrastructure and operations, and data and analytics. Each domain reveals specific gaps that will either accelerate or stall your implementation.
The GDHP framework, used by health ministries globally, scores organizations on these domains before any implementation begins. This matters because a hospital with strong infrastructure but weak data governance will hit a wall the moment it tries to scale analytics across departments. Knowing your baseline prevents that wall from appearing mid-project.
In the Middle East specifically, national interoperability alignment is not optional. Platforms like Abu Dhabi's Malaffi and Dubai's NABIDH are government-mandated health information exchanges. Any digital solution you implement must connect to these systems or risk being isolated and non-compliant. Building a solid digital strategy for healthcare leaders means treating interoperability as a foundational requirement, not an afterthought.
Here is a practical readiness checklist to run before your next project kickoff:
- Leadership alignment: Has your C-suite formally endorsed the digital health roadmap?
- Infrastructure audit: Are your networks, servers, and devices capable of supporting new platforms?
- Data readiness: Is patient data structured, clean, and accessible for analytics?
- Regulatory mapping: Have you documented compliance requirements for Malaffi, NABIDH, or Saudi MOH systems?
- Change management plan: Is there a dedicated team to manage staff adoption and training?
- Vendor due diligence: Have vendors demonstrated regional compliance experience?
| Readiness domain | Key question | Risk if skipped |
|---|---|---|
| Leadership and policy | Is executive sponsorship confirmed? | Low adoption, stalled rollout |
| Infrastructure | Can systems handle new load? | Performance failures at scale |
| Data and analytics | Is data clean and accessible? | Inaccurate outcomes, poor decisions |
| Regulatory alignment | Are mandates mapped to solution design? | Non-compliance, project shutdown |
Pro Tip: Involve your clinical informatics lead, IT director, and a government affairs contact in the readiness assessment from day one. Cross-functional buy-in at this stage cuts approval timelines by weeks and surfaces blockers before they become crises.
For a deeper look at how to structure this phase, the efficiency boost tips from our 2026 guide offer region-specific prioritization frameworks.
Choosing the right frameworks: Structured approaches for success
Once readiness is confirmed and leadership is aligned, the next question is: how do you actually structure the implementation? This is where most organizations either gain a significant advantage or lose months to confusion and rework.
Two frameworks dominate healthcare digital implementation globally. The Consolidated Framework for Implementation Research, known as CFIR, guides teams by assessing determinants across five domains: intervention characteristics, outer setting, inner setting, individuals involved, and implementation processes. Digital maturity models, by contrast, focus on scoring current capabilities and mapping a progression path. Both are valuable. The choice depends on whether your primary challenge is adoption (use CFIR) or capability building (use a maturity model).
| Framework | Best for | Core strength | Limitation |
|---|---|---|---|
| CFIR | Adoption and behavior change | Identifies why implementations fail | Requires trained facilitators |
| Digital maturity model | Capability planning | Clear progression benchmarks | Less focused on human factors |
| Hybrid approach | Complex, multi-site rollouts | Covers both capability and adoption | Higher planning overhead |
A structured stepwise approach works best for real-world projects. Here is how leading teams apply it:
- Study design: Define the problem, scope, and success metrics before selecting technology.
- Data collection: Gather baseline data on current workflows, patient volumes, and system performance.
- Framework application: Map your project against CFIR domains or maturity benchmarks to identify gaps.
- Pilot execution: Run a controlled pilot in one department or facility with clear feedback loops.
- Analysis and interpretation: Measure outcomes against baselines. What worked? What did not?
- Dissemination: Share results internally and with regulatory bodies. Scale what works.
Structure reduces overlooked risks. Without a framework, teams routinely underestimate the outer setting, which includes government regulations, payer requirements, and community factors. In the Middle East, this outer setting is unusually active, with ministries issuing new digital health directives regularly. A framework forces you to account for this.
Our IT modernization guide covers how UAE businesses are applying these structured approaches to legacy system upgrades with measurable results.
Pro Tip: Assign a named framework lead to each implementation domain. When everyone is accountable for everything, nothing gets owned. One person per domain creates clear responsibility and faster escalation when issues arise.
Executing implementation: Best practices and common pitfalls
Structured planning is essential, but strong execution makes or breaks digital health initiatives. Here is how leading organizations in the region are achieving measurable impact.

The evidence from Saudi Arabia is striking. Seha Virtual Hospital scaled telemedicine visits from 1,717 in 2021 to 27,896 in 2024, with high patient satisfaction scores. That is not luck. It is the result of phased rollout, cross-team coordination, and continuous data-driven refinement. In a separate initiative, a medication refill digital system improved patient adherence from 35% to 79%, reduced medication oversupply from 50% to 19%, and cut refill wait times from 40 minutes to just 5 minutes.
These results share a common pattern: they started with a high-impact, well-defined problem, used data to guide every decision, and invested heavily in staff training.
Key best practices for execution:
- Start with high-impact areas: Choose workflows where digital tools will immediately reduce bottlenecks or errors.
- Run phased pilots: Test in one unit before scaling. Pilots surface integration issues without disrupting the whole organization.
- Leverage analytics for patient outcomes: Build feedback dashboards from day one so teams can see what is working in real time.
- Invest in ongoing training: Budget for training as a recurring cost, not a one-time event.
- Adapt to local workflows: A solution that works in Europe may need significant redesign for Gulf clinical environments.
Common mistake to avoid: Organizations consistently underestimate training needs. A new electronic health record or telemedicine platform is only as effective as the clinicians using it. Allocate at least 20% of your implementation budget to change management and training. Skipping this step is the single most common reason digital health projects underperform.
The role of AI in healthcare is growing fast in the region, but AI tools require even more rigorous change management than standard software. Clinicians need to understand what the system is recommending and why before they will trust it in patient-facing decisions.
Securing outcomes: Data governance and trust architecture
Reliable outcomes and scaling depend not just on smart technology and process, but on trust and security from the very start.
Trust architecture is the foundation for scaling AI and precision medicine across healthcare systems. Security and governance must be embedded before clinical integration begins, not retrofitted afterward. This is a lesson many organizations learn the hard way.
The financial stakes are real. Healthcare data breaches cost organizations over USD 10 million on average, and regulatory compliance in the UAE and Saudi Arabia is non-negotiable. Both countries have active health data protection frameworks, and violations carry serious operational and reputational consequences.
The hidden cost of weak governance: A data breach in a healthcare setting does not just cost money. It erodes patient trust, triggers regulatory audits, and can halt digital programs entirely. Organizations that treat governance as a checkbox exercise rather than a strategic function pay this price repeatedly.
Actions for building a trusted architecture:
- Adopt security-by-design: Embed access controls, encryption, and audit trails into system architecture from the start.
- Map to local regulations: Align with UAE's HAAD/DHA data policies and Saudi Arabia's PDPL and MOH digital health guidelines.
- Conduct regular penetration testing: Do not wait for a breach to find vulnerabilities.
- Establish a data stewardship committee: Assign ownership of data quality, access, and compliance across departments.
- Minimize shadow AI risk: Inventory all AI tools in use, including those adopted informally by clinical staff, and bring them under governance oversight.
For a practical checklist on protecting patient data, our data security steps guide covers the specific requirements Middle East healthcare organizations face in 2026. You can also explore health data privacy policies at the policy level for broader regulatory context.
Pro Tip: Establish your data governance committee before you scale any pilot regionally. Governance gaps that are manageable in a single-site pilot become serious liabilities when you are operating across five hospitals in three emirates.
Why focusing on interoperability and trust drives long-term impact
After working through the technical and operational factors, it is worth stepping back to address what most implementation guides quietly avoid: the difference between organizations that sustain digital health gains and those that plateau after the first pilot.
The answer is almost always interoperability and trust, not technology selection. Malaffi and NABIDH are not just compliance requirements. They are force multipliers. When your systems connect to a regional health information exchange, every new tool you add benefits from shared patient history, reduces duplicate testing, and improves care coordination across providers. One-off solutions, no matter how well built, cannot replicate that network effect.
The hidden cost of overlooking trust architecture is equally significant. We have seen organizations invest heavily in AI's role in digital transformation only to face clinician resistance because the governance framework was not in place to explain how the AI made decisions. Trust is not a soft concept. It is a measurable operational variable.
Sustainable digital health in the Middle East comes from government alignment, ongoing data stewardship, and executive accountability working together. Leaders who invest in this groundwork consistently outperform those chasing the newest tool. The technology matters less than the system you build around it.
Partnering for digital health implementation success
Seeing what works in the region is one thing. Having the right team to execute it is another.
YS Lootah Tech brings Dubai-based expertise in application development services and AI and machine learning solutions specifically designed for regulated, high-stakes environments like healthcare. Our teams understand Malaffi, NABIDH, and the compliance landscape across the Gulf. Whether you are building a telemedicine platform, a patient analytics system, or a secure health data exchange, we help you avoid the implementation pitfalls covered in this guide. Explore how YS Lootah Tech can accelerate your digital health roadmap with solutions built for the region from day one.
Frequently asked questions
What is the most important factor in digital health solution implementation in the Middle East?
National alignment and interoperability are the most critical factors. Platforms like UAE's Malaffi and Dubai's NABIDH enable coordinated, scalable implementation that isolated solutions simply cannot achieve.
How can organizations evaluate their readiness for digital health projects?
Digital maturity assessments cover leadership, policy, infrastructure, and data analytics to surface specific gaps before implementation begins, preventing costly mid-project surprises.
Why is trust architecture essential in digital health?
Trust architecture ensures security and governance are embedded from the start, which is the only way to safely scale AI tools and precision medicine into clinical workflows without exposing patients or the organization to unacceptable risk.
What measurable impacts have digital health projects achieved in the region?
Saudi initiatives delivered dramatic results: medication adherence improved from 35% to 79%, while telemedicine visits scaled from 1,717 in 2021 to 27,896 in 2024, demonstrating what structured, data-driven implementation can achieve.